The goal of this study was to assess knowledge and beliefs concerning climate change and infectious diseases in Bangladesh and to recommend One Health policies to reduce the burden of infectious diseases as related to climate change. To reduce the harmful effects of climate change on infectious diseases, it is crucial to consider Bangladesh’s capability to address the present and future challenges as related to infectious disease prevention and control [11, 15, 17, 35]. Collectively, the study results show that most respondents surveyed had a generally low knowledge of climate change and the influence of climate change on infectious diseases. Lack of education was associated with poor knowledge about infectious diseases, a finding that aligns with similar studies conducted in China and Nepal [39, 40]where the respondents demonstrated low knowledge of climate change and infectious diseases. Social and economic factors such as lower SES and inadequate public health training were consistently associated with reduced awareness in vulnerable communities across these contexts [39]. As SES remains a key determinant of knowledge, future efforts should focus on addressing these disparities to reduce the burden of climate-sensitive infectious diseases in Bangladesh.
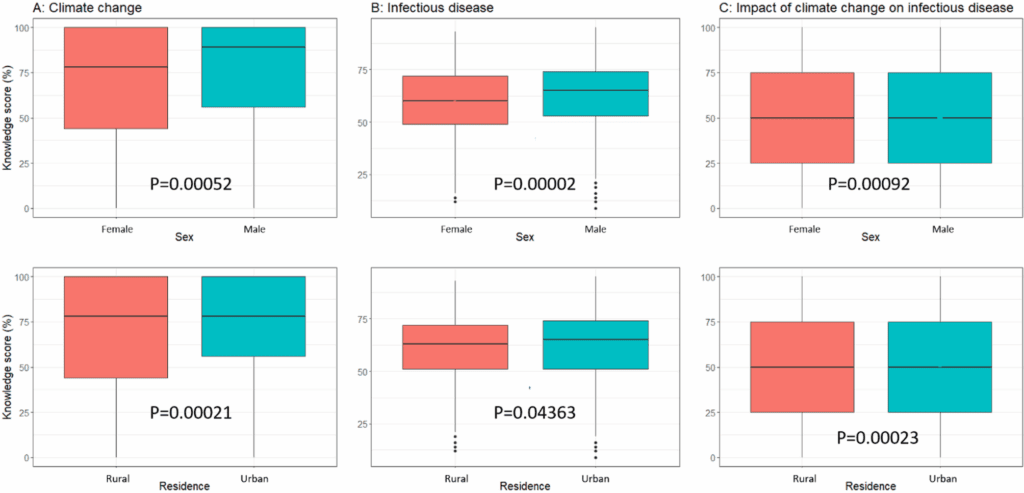
Our study additionally indicated that when compared to rural respondents, urban respondents were more knowledgeable about infectious diseases and climate change. The finding related to infectious disease is consistent with a previous study conducted in Bangladesh [16] and can be attributed to the difference in education level among the urban versus rural respondents. The finding that urban participants have greater knowledge than rural is also closely aligned with other studies conducted in Bangladesh [16, 20, 41] and Northeast Ethiopia, where respondents’ awareness of climate change and its health effects was limited due to insufficient community-level training [42]. Our study finding that overall educated respondents were more knowledgeable on the topics of climate change and infectious disease is also in line with other studies [40, 43, 44] and may be due to their ability to comprehend information and read and increased engagement with the internet, social media, television, and books to collect information. People’s education level in northern Bangladesh is greatly influenced by the challenges posed in rural and remote areas, where socioeconomic disparities associated with geographic location may contribute to the differences in knowledge among urban versus rural respondents [45, 46]. Diversity in socioeconomic position was also considered in a previous study from Singapore to examine the knowledge gap hypothesis on the issue of climate change [46].
Furthermore, our findings support that compared to male respondents, female respondents were less knowledgeable about the impact of climate change on infectious diseases. This can be explained by women in Bangladesh being, on average, less educated, particularly in rural areas [47, 48]. Strategies such as providing more and better access to education, particularly for rural women, along with policy participation and inclusion, and access to resources, can position women as local advocates for healthier communities. Thus, gender-sensitive educational initiatives can play a critical role in improving awareness and strengthening community-level adaptive capacity. Identifying and addressing gaps in people’s knowledge of infectious diseases and their association with climate change is essential for enhancing community adaptive capacity. Several studies conducted in various countries, including China, Egypt, and Indonesia, have investigated people’s knowledge of climate change and its impact on health [31, 49, 50]. This study is the first to be carried out in Bangladesh to assess knowledge and beliefs regarding climate change and various infectious diseases. In Bangladesh, beliefs regarding climate change and infectious disease outbreaks are shaped by a complex mix of sociodemographic factors [51, 52]. Education, SES, urbanization, age, gender, and cultural context all interact to produce distinct patterns of knowledge and belief [51, 52]. Understanding these clusters is essential for designing effective public health interventions and communication strategies that resonate with diverse segments of the population. However, our findings can serve as a foundational reference for a future cohort study, enabling policymakers to develop initiatives and advocacies to improve the knowledge about the impact of climate change on infectious diseases. The findings of this study can also help policymakers, service providers, and other stakeholders build effective plans for preventing and controlling climate-sensitive infectious diseases.
Bangladesh’s population is becoming increasingly aware of the links between climate change and risks of infectious/insect-borne diseases. However, this knowledge has not translated into high policy priority or robust infection control measures [18]. The reasons are multifaceted: deficiencies in data and surveillance, competing health priorities, inadequate health systems, socioeconomic vulnerabilities, disjointed policy responses, and insufficient cross-sectoral integration [18,19,20]. To rectify this disparity, Bangladesh necessitates improved disease surveillance and data integration, investment in resilient health systems and infection prevention and control infrastructure, cross-sectoral policy integration and coordination, targeted public education and behavior modification initiatives, and the integration of climate adaptation into infection control and public health strategies.
Additionally, the study results have implications for the One Health approach and policies. Results support the need for government decision-making to be based on the concept of One Health approach. The One Health concept speaks for the inseparability of human, animal, and environmental health through an integrated vision of health care and is gaining global recognition to combat health concerns based on human-animal-environment interactions, particularly zoonotic diseases [4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54]. In Bangladesh, adopting the One Health approach can strengthen resilience and support sustainable strategies in addressing climate change challenges and infectious diseases. Existing national programs such as the Communicable Disease Control unit (DGHS), the Department of Livestock Services, and the Ministry of Environment, Forest and Climate Change provide institutional frameworks that could be leveraged for integrated implementation. For example, Bangladesh can make use of local communities and engage them in participating in disease education and prevention efforts about climate change and infectious diseases. Community-based participation can focus on education campaigns throughout schools, villages, and communities, as well as on involving community politicians, leaders, religious figures, and women’s groups. Finally, the findings of this study support that increased awareness of climate change and infectious diseases can be achieved through increasing the general education level of the population, practical training, school educational campaigns and community-level health systems in northern Bangladesh. There must be proactive implementation of public health decisions and necessary adaptive strategies to be effective. Practical and solid forecasting can provide direction for government policies and social behaviors, which are essential for addressing issues related to climate change, including population displacement, increased urbanization, and poor sanitation. Establishing direct associations between adverse weather events and communicable diseases is also necessary. Finally, weather-based early warning systems can be developed to improve monitoring and forecast the risk of disease outbreaks. For example, rainfall monitoring linked to seasonal dengue outbreaks can inform early warning systems and targeted public health interventions [25, 55].